This weeks post will consider the patient with inflamed legs. It’s a subject that whilst not entirely thrilling, is brimming with myth, legend and here say galore. So….. it is my hope that we can put a lot of this illogical nonsense to bed.
Broadly speaking inflamed legs will have at least 1 of these 3 underlying causes, but of course multiple disease processes can co-exist.
- Peripheral vascular insufficiency
- Infection
- Thromboembolism
Myth 1. Chronic cellulitis is a thing isn’t it? No it isn’t! Heres why.
Skin infections are associated with a greater risk of morbidly and mortality than a great many infections, so what usually happens is that the patient will develop cellulitis for example and will either resolve spontaneously (or more likely with 1-2 weeks of antibiotics) or the infection gets worse, they develop sepsis and die. It makes little logical sense that a serious infection (serious in the sense that it requires treatment) is able to persist for weeks- months without requiring lengthy hospital stay or resulting in eternal sleep. Chronic yes. But what you’re likely looking at is something that isn’t cellulitis. Probably venous eczema or lipodermatosclerosis to be precise. So if you’re about to prescribe week 13 of oral antibiotics for ‘chronic cellulitis’, STOP. DON’T!
Myth 2. Bilateral cellulitis. (Not a complete myth, but unlikely, so you need to think of something else).
What you are letting yourself believe here is that two separate sources of infection have occurred in both legs spontaneously at the same time. Whilst this is by no means impossible, it is however rather unlikely, and such a picture probably points to an alternative diagnosis. Venous eczema and or lipodermatosclerosis. You’re probably starting to see a pattern here.
If the leg inflammation is chronic, and or bilateral, then it is probably caused by peripheral vascular insufficiency.
Lipodermatosclerosis (aka sclerosing panniculitis, hypodermitis sclerodermaformis)
This is a fairly common problem that you’ve seen plenty of times even if you didn’t realise that it has a name. It is a chronic inflammatory skin condition secondary to chronic venous insufficiency that results in venous hypertension in the legs. Subsequently, leukocyte migration from the veins occurs and initiates the inflammatory cascade in the surrounding subcutaneous tissues (which doesn’t stop). The result is fibrosis and hardening of the skin on the lower legs which will develop a nodular feel and appearance. Pain and poor wound healing is a major problem and will often lead to venous ulceration that is difficult to treat.
Lipodermatosclerosis is usually seen from middle age onwards, is far more prevalent in women, those who are sedentary or obese. It exists chronically (see below) with narrowed ankles, swollen calfs (inverted champagne bottle appearance) and hyper pigmented or blanched avascular areas of skin. In acutely inflamed episodes it can mimic cellulitis to the unwary clinician.
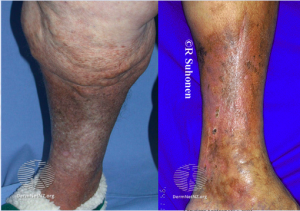
Chronically, lipodermatosclerosis can be effectively managed by encouraging physical activity and weight loss (if obesity is a factor), regular analgesia, compression hosiery (once arterial insufficiency has been excluded by doppler) and concurrent management of eczema (emollients and topical steroids) will all be beneficial. There are pharmacological interventions that can be beneficial but are likely to be instigated by dermatology or vascular services in secondary care if the primary care management doesn’t adequately control symptoms or the disease continues to progress.
Acute Lipodermatosclerosis
It isn’t the case that lipodermatosclerosis develops acutely, rather that there is an acute inflammatory element on top of the pre existing chronic phase. This will usually be seen as bilateral lower leg inflammation (unilateral is possible but far less likely) that may be painful, swollen, uncomfortable but the patient is nearly always well (unless other acute illness coexists). During intercurrent systemic illness (e.g viral illness) the legs will often acutely inflame in response to wider spread inflammation.
There is often venous eczema concurrently and may be the reason the an acute phase response. Managing both should help to promote recovery to baseline.
If localised skin infection is the cause of the acute flare then this should be treated with antibiotics but remember that infection is more likely if unilateral leg or localised inflammation is present. Infection, namely cellulitis is very unlikely if the inflammation is bilateral (I may have already mentioned this once or twice).
Infection
Skin infection will manifest itself according to its depth. Whether superficial (impetigo or impetiginised eczema), dermal (erysipelas) or cellulitis (subcutaneous adipose tissue involved).
Impetigo on varicosed eczema may present at first glance as an acute eczematous flare up, but you may noticed pustular lesions or crusting that would suggest concurrent infection. Manage with topical steroids and antibiotics (topical or systemic depending on spread/ severity and local guidance).
The patient with cellulitis or erysipelas (essentially a superficial version of cellulitis) will always need systemic antibiotics, with hospital admission if they are unwell or at high risk of sepsis (i.e fever, treatment failure, septic, consider admission if immunocompromised or suppressed). Whilst cellulitis most commonly occurs on the lower leg, it may occur anywhere, especially when the skin integrity is compromised (wound, dry skin conditions etc).

Venous thromboembolism and thrombophlebitis will be discussed in next weeks blog so keep your eye out for this.
References
https://dermnetnz.org/topics/lipodermatosclerosis/
https://cks.nice.org.uk/topics/venous-eczema-lipodermatosclerosis/management/management/[/vc_column_text][/vc_column][/vc_row]




